Profiles In Nursing
Alice Magaw Kessel (1860-1928), Pioneering Nurse Anesthetist
She performed 14,380 procedures with no fatalities
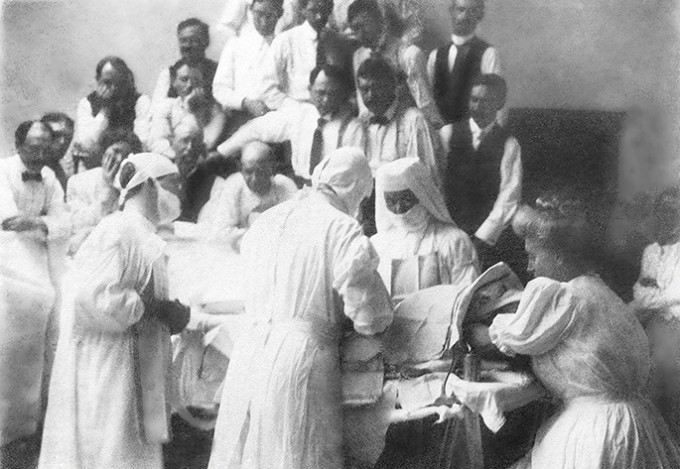
Around the turn of the last century, nurse anesthetist Alice Magaw and her longtime friend Edith Graham Mayo forever changed both anesthesia practice and physicians’ attitudes toward nurses who administer anesthetics.
Graham and the Mayo Brothers
Born in Ohio shortly before the Civil War, Alice Magaw grew up in Michigan and moved with her family to Rochester, Minn., in her early 20s. There, she met and befriended Edith Graham, who later became her classmate in the nursing school at Chicago Hospital for Women and Children.
When they graduated in 1889, Magaw remained in Chicago as a private duty nurse while Graham returned to Rochester and went to work at the newly established St. Marys Hospital as a nurse for surgeons Charles H. and William J. Mayo. When they graduated in 1889, Magaw remained in Chicago as a private duty nurse while Graham returned to Rochester and went to work at the newly established St. Marys Hospital as a nurse for surgeons Charles H. and William J. Mayo.
At the suggestion of their father, surgeon William W. Mayo, the Mayo brothers trained Graham to become what they originally called an “anaesthetizer”: a highly skilled nurse who would administer ether and other anesthetics to surgical patients. Graham was the Mayos’ first nurse anesthetist and received considerable credit for minimizing the new hospital’s surgical mortality rate.
In April 1893, after more than 650 surgeries, Graham retired to marry Charles Mayo. The Mayos hired Magaw as her successor.
Talking Them to Sleep
The most common anesthetics at that time were nitrous oxide, chloroform and ether. The Mayo brothers strongly preferred ether, which was less pleasant but more effective than nitrous oxide and much safer than chloroform. Magaw once remarked, “ether kills slowly, giving plenty of warning, but with chloroform there is not even time to say good-bye.”



