Feature
Nursing on the Front Lines of COVID-19
Keeping the virus (and panic) under control at the Seattle-area hospital that treated the first U.S. case
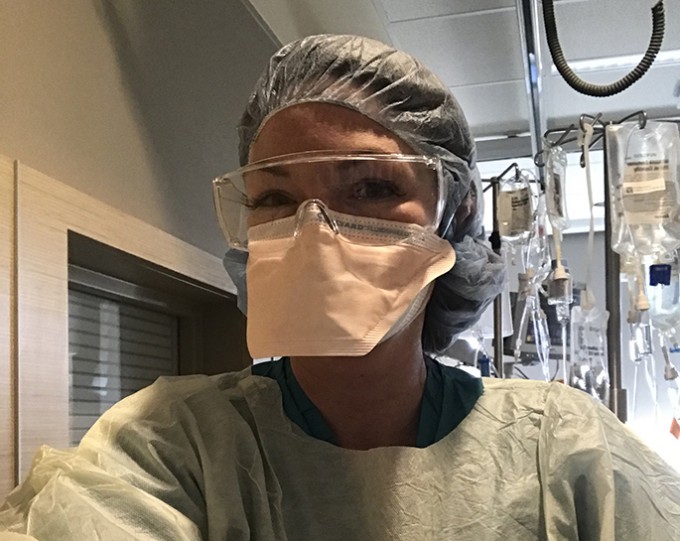
I have never been particularly “germ-averse.”
While I’m a protocol-following professional at work, I can be a bit laissez-faire about pathogens in my personal life. I’m not the type of nurse to shed my scrubs and change my shoes like Mr. Rogers as soon as I arrive home. I never required a post-shift shower before hugging and kissing my kid. Working in acute care for over 18 years has led to a sense of invincibility when it comes to communicable diseases.
Until now.
I work at Providence Regional Medical Center Everett, in Everett, Wash., which had the dubious honor of becoming the first hospital in the U.S. to care for a patient with the 2019 novel coronavirus disease, abbreviated 2019-nCoV or just COVID-19. This is my experience of these scary first weeks.
Noise
My patient’s ventilator alarms blare loudly, despite being partially muffled by a tightly sealed door. This door is part of a system designed to generate a negative airflow space for patients with highly infectious respiratory diseases such as COVID-19, which my patient may or may not have. At least another 48 hours will pass before results are available, but in the meantime, we are treating this case with the utmost regard for transmission prevention.
Although the alarm is urgent — “circuit disconnection” — and my patient may momentarily not receive adequate oxygen, it’s going to take significantly longer than the standard few seconds for me to get to the bedside and reconnect. Whole minutes might pass before I’ve put on my personal protection equipment (PPE) and am prepared to provide care.
First, I don a yellow gown over my hospital-provided disposable scrubs and attach a battery pack to my waistband. Next, I pull not one but two sets of gloves over my hands; the outer pair is more typically used for handling hazardous drugs such as chemotherapy.













